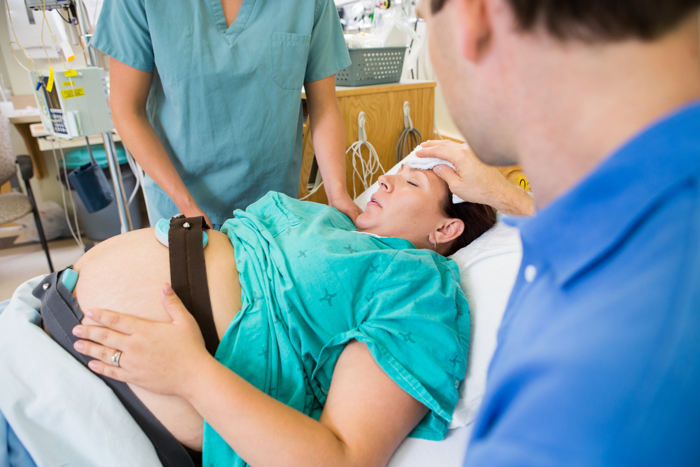
Signs that labour has started
The start of childbirth, labour and how you experience giving birth is very individual. No two births are the same, so having a second baby may be different to the first time.
Most births start naturally (spontaneously) between gestational week 37 and 42. Labour typically starts when the uterus (womb) starts tightening to produce contractions, but you may also experience other signs that you are going into labour.
Contractions
Contractions are painful cramps that come more frequently than every 10 minutes or so and last for 45-60 seconds.
Contractions usually come several minutes apart. They last a short time at the start, and as labour progresses they increase in frequency, duration and intensity. Most women feel the pain in their lower belly and/or lower back.
Time your contractions, and phone the hospital/unit when they are regular or about 5-6 minutes apart.
If you are a long way from the hospital, have given birth very fast before, had complications in previous pregnancies or births, or if you are worried, phone the hospital when the contractions start.
The stages of childbirth
Once labour has started, the contractions change your cervix so it begins to open to make space for your baby to pass through the birth canal.
The birth canal consists of:
- The pelvis – the bony part of the birth canal
- The muscles in the pelvis
- The vagina – the soft part of the birth canal
The pelvis is funnel-shaped, so its size differs at the different levels of the pelvis. This means that the baby has to make some rotations during labour to adapt and pass through the pelvis.
Three stages
Labour is divided into three stages: the dilation stage, expulsion stage and placental stage. The dilation (opening) stage is the longest, while the expulsion (pushing out) stage lasts 30-60 minutes, and the placental stage takes from a few minutes to up to 60 minutes.
Various factors influence how long it takes to give birth:
- Whether you've given birth before or not. Giving birth to a first baby usually takes the longest.
- The frequency and effectiveness of your contractions influence how long the labour lasts. Regular and effective contractions are all-important for good progress; the contractions push the baby down into the pelvis and the cervix (neck of the womb) opens.
Active labour in first-time mothers lasts 4 to 16 hours. For women who have given birth before, labour usually lasts 2 to 11 hours. This varies from woman to woman and from birth to birth.
Dilation stage
The first stage of labour is called the ‘dilation stage’. At this stage, the cervix (neck of the womb) has to open to let the baby pass down into the pelvis and be delivered.
The cervix changes from being closed to being 10 cm open (fully dilated). Not until the cervix is fully dilated, can the baby be delivered.
As the cervix dilates, there will be some blood-tinged vaginal discharge, known as the ‘bloody show’. This is a sign that the cervix is dilating under the effects of the contractions and the pressure from the baby’s head. Your waters may break at any stage of labour, but usually this happens in the active phase of the dilation stage.
Latent phase – first part of the dilation stage
The first part of the dilation stage, the latent phase, is the longest phase of labour. This phase starts from when you have regular contractions less than 10 minutes apart. The contractions are spaced far apart to begin with, but they gradually increase in strength and come at shorter intervals.
When the cervix is about 4-5 centimetres dilated, labour transitions to the active phase. The contractions become more effective and the cervix dilates (opens) faster.
Examinations
The midwife checks the progress of labour by examining your belly to assess your contractions. By an internal exam, the midwife can check how dilated the cervix is and how the baby’s head is positioned in the birth canal.
It is not uncommon to have examinations several times during labour, and you will be informed of this before it is done. The midwife will also tell you how your labour is progressing.
Activity and rest during labour
During the dilation stage, you should switch between activity and rest. Your movement and activity help your baby to rotate and pass through the pelvis. Most persons also find the contractions less painful if they are active than if they are lying still in bed. The midwife will help you switch between comfortable resting positions and being active.
During the dilation stage, one of the main tasks of the midwife is to help you find positions that aid your baby’s passage down through the pelvis and birth canal. At this stage of labour, the midwife wants you to use the force of gravity and keep moving while still relaxing your body.
Labour takes a lot of energy. So, you need to boost your body’s energy levels by drinking and eating light meals. You will be offered food and drink.
Expulsion stage
You will now be using each contraction to push out your baby. Combined with the force of the contractions, you will be pushing your baby, contraction by contraction, down into your vagina and out. You will need to find birthing positions that allow you to push when the next contraction comes, and then to rest between contractions.
It is often helpful to vary between different birthing positions in this phase of labour. This helps your baby to rotate and pass downwards in the pelvis. The midwife will help you find birthing positions that work for you and help labour to progress.
The midwife will tell you how you to push when the baby’s head and body are about to be delivered. You and the midwife will need to work as a team now, so that the birth is as gentle on the baby as possible, and to prevent you tearing. The midwife will support the tissue between your vagina and anus (perineum) while the baby’s head and body are born.
Labour pains
The pains of labour are caused by the uterus (womb), which is a large muscle, contracting, which causes your muscles, sinews and nerves to be stretched and squeezed. The pain changes in strength, duration and location as labour progresses.
At the start, the contractions come a few minutes apart, and towards the end, they are more frequent and more painful. Most women have pauses in between where they have no pain, and this is where you can take a breather and brace yourself for the next contraction.
When your baby passes through the birth canal, you will feel the pressure against your tissue and nerves. Just before you give birth, the pressure from your baby will cause pressure and tightening in your vagina and against your rectum. This triggers a strong urge to push.
Labour pains are experienced very differently from one person to the next. Each person faces childbirth with her own situation, previous impressions, experiences and cultural background. This may influence how you react to the pain of being in labour.
The offer of pain relief may vary, and not all types of pain relief are available at all hospital maternity wards. Talk to the midwife or GP at your antenatal check-ups about what is available at the hospital where you are booked to have your baby.
After your baby is born
Your baby has been born, but delivery is not quite over yet. The afterbirth (placenta and foetal membranes) also has to come out. This usually happens shortly after the baby is born, or within about 60 minutes. The placenta and the foetal membranes are released from inside the uterus.
When the placenta comes away, you may feel a weak contraction and there may be some vaginal bleeding. When the placenta has come away inside, you have to push it out just like you did when you gave birth to your baby. This may cause a bit of discomfort, but does not hurt.
Where the placenta was attached to the uterus, there will be a wound. It is important that the uterus now contracts to prevent heavy bleeding. After you have given birth, the midwife also has to check for any tears inside the birth canal. If any tears need stitches, you will be given local anaesthetic. The thread used for placing the stitches dissolves by itself, so the stitches do not have to be removed.
As soon as your baby is born, he or she will be placed in your arms. After being born, babies start seeking out their mother’s breast. It is important that the baby and you, the father, the co-mother or a helper have quiet time together without any disruption. That is why it is good to wait a while before using a mobile phone.
You will need to take it easy after going through labour and all those emotions. Your baby needs peace and quiet and your undivided attention to find your breast and feed for the first time. This is an important time and should not be needlessly disturbed.
After childbirth
The length of time spent in hospital after giving birth is individual and adjusted to your and your baby needs. After a caesarean section, you are usually hospitalised for 3-4 days.
The midwife examines the baby immediately after the birth. Within the first few days after the birth, your baby will be examined by a paediatrician. It is a good idea to have one of the parents present.
During the paediatrician's examination, you can ask questions and raise any issues you think it is important for the paediatrician to be aware of. Before going home, you will receive information about who to contact, and how to do so, if you should need advice or assistance after you are back home with your baby.
The aim of postnatal care is, as far as possible, to individualise it to your needs.
If you do not go into spontaneous labour
The aim of all antenatal care is to promote natural childbirth. Labour that starts spontaneously between gestational week 37 and 42, in a healthy mother after an uncomplicated pregnancy, is best for the mother and baby. But this does not happen for everyone. There may be factors in both the mother, the baby or both that make it safest to get childbirth started.
Igangsetting av fødselen
Labour is only induced after a thorough assessment and when it is in the best interest of the mother and/or child.